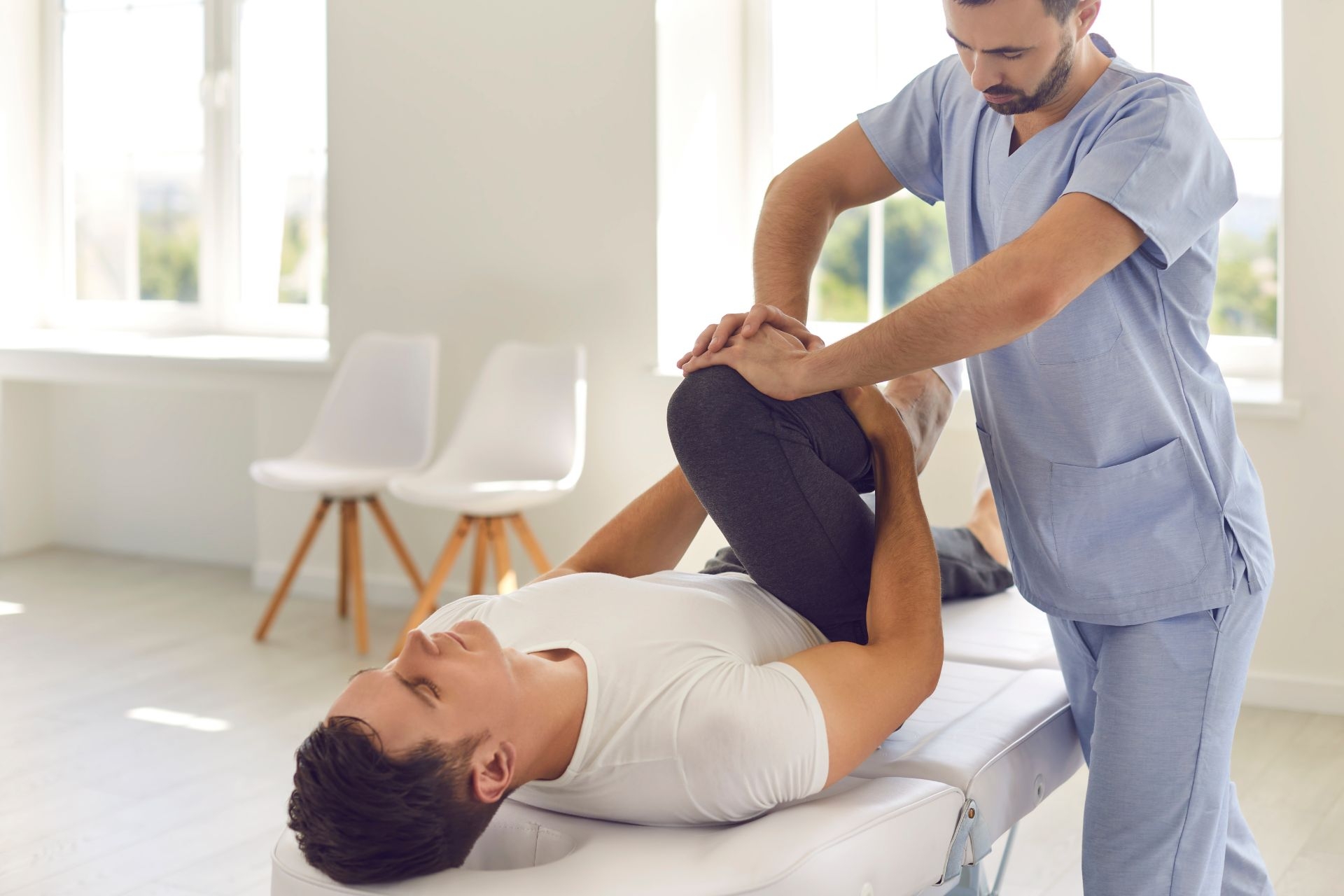
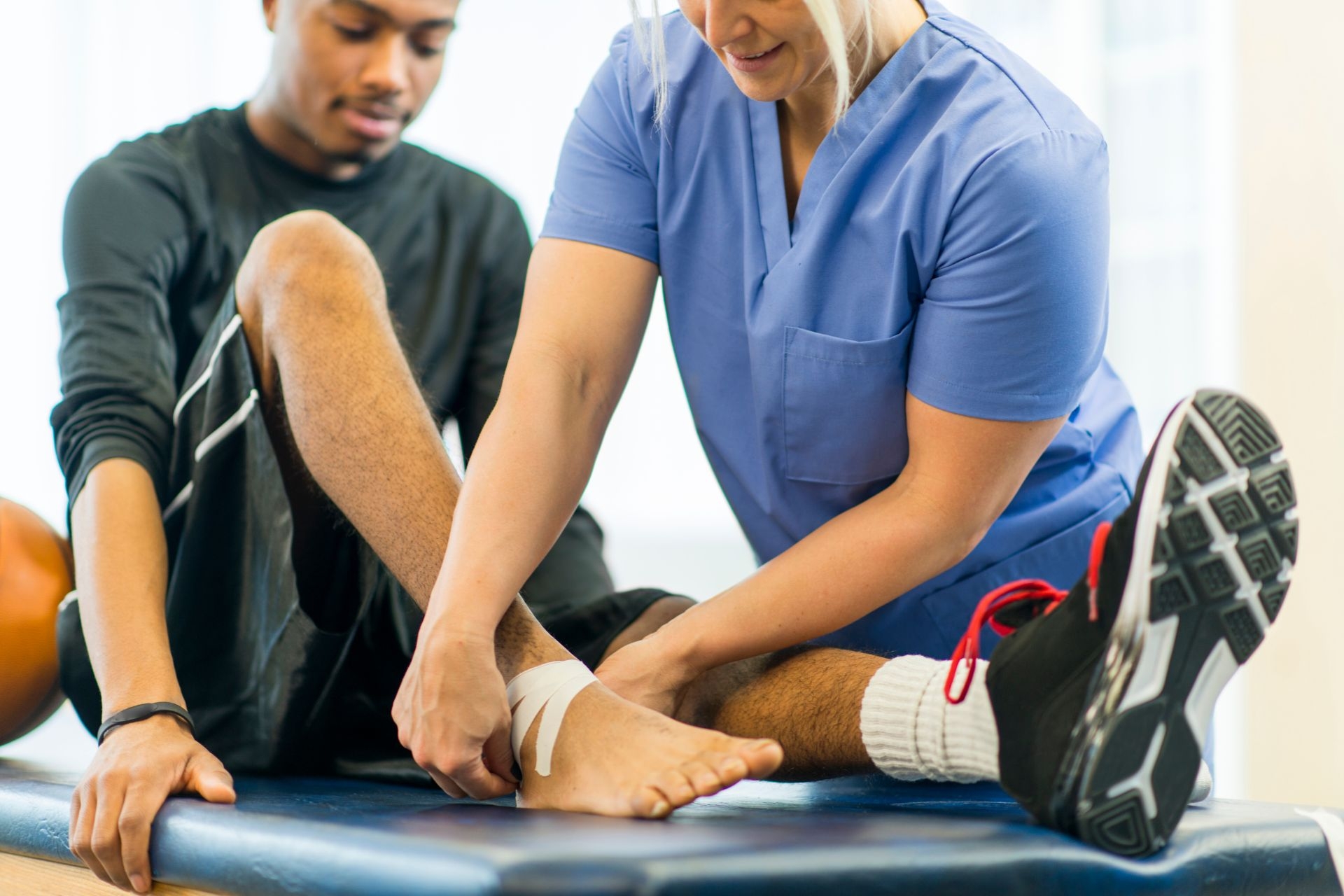
Soft Tissue Mobilization
How does soft tissue mobilization help with breaking down scar tissue?
Soft tissue mobilization helps with breaking down scar tissue by applying specific pressure and movement techniques to the affected area. This helps to realign collagen fibers and break up adhesions that form as a result of the body's natural healing process. By breaking down scar tissue, soft tissue mobilization can improve flexibility, reduce pain, and restore normal function to the area.